|
Case Report
A case of myelodysplastic syndrome with extramedullary hematopoiesis followed by rapid transformation into NRAS-mutated acute myeloid leukemia in an orthotopic liver transplant recipient
1 MD, Assistant Professor, Department of Medicine, Division of General Internal Medicine, Rutgers New Jersey Medical School, Newark, NJ, USA
2 MD, Resident Physician, Department of Medicine, Rutgers New Jersey Medical School, Newark, NJ, USA
3 MD, PhD, Assistant Professor, Department of Pathology and Laboratory Medicine, Division of Hematopathology, Rutgers Robert Wood Johnson Medical School, New Brunswick, NJ, USA
4 DO, Fellow, Department of Medicine, Division of Gastroenterology and Hepatology, Rutgers New Jersey Medical School, Newark, NJ, USA
5 MD, Assistant Professor, Department of Medicine, Division of Hematology and Oncology, Rutgers New Jersey Medical School & Rutgers Cancer Institute, Newark, NJ, USA
Address correspondence to:
Ravi Upadhyay
90 Bergen Street, Suite 4200, Newark, NJ 07103,
USA
Message to Corresponding Author
Article ID: 100139Z10RU2024
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Upadhyay R, Shah M, Serei V, Panchal D, Shah A. A case of myelodysplastic syndrome with extramedullary hematopoiesis followed by rapid transformation into NRAS-mutated acute myeloid leukemia in an orthotopic liver transplant recipient. J Case Rep Images Oncology 2024;10(2):31–36.ABSTRACT
Introduction: With the increase in lifespan and the resulting immunosuppression that decreases tumor surveillance, secondary malignancies in liver transplant recipients are becoming more common.
Case Report: We present a unique case of a 33-year-old man who developed myelodysplastic syndrome with transformation into acute myeloid leukemia following orthotopic liver transplantation. Approximately 18 months after the patient’s liver transplantation, he developed leukopenia and neutropenia which shortly progressed into leukocytosis with peripheral blasts. His bone marrow aspirate showed 10% myeloblasts with the patient thereafter being diagnosed with myelodysplastic syndrome with excess blasts-2. Two months later, the patient had repeat flow cytometry of his blood which revealed 18% myeloblasts in the CD45 dim blast gate along with co-expression of CD34 and CD117, consistent with a diagnosis of refractory anemia with excess of blasts in transformation/acute myeloid leukemia. Next generation sequencing exhibited one variant of strong clinical significance in the neuroblastoma RAS viral oncogene homolog. The patient was not a candidate for allogenic stem cell transplantation and he expired approximately five months after diagnosis of acute myeloid leukemia despite two cycles of decitabine and venetoclax.
Conclusion: This case demonstrates how complications of orthotopic liver transplantation including secondary malignancies are becoming more common and that the benefits and risks associated with chronic immunosuppressive therapy must be balanced against each other. The case also exhibits the heterogeneous nature of this phenomenon and that further work is needed to determine the optimal treatment for this post-liver transplant disease which unfortunately heralds a poor prognosis.
Keywords: Acute myeloid leukemia, Extramedullary hematopoiesis, Myelodysplastic syndrome, NRAS, Orthotopic liver transplantation
Introduction
Development of myelodysplastic syndrome (MDS) and acute myeloid leukemia (AML) is a rare phenomenon after orthotopic liver transplantation (OLT). It is thought that the use of immunosuppressive drugs after transplantation increases the risk of malignancy, in general [1]. Compared to more common malignancies after solid organ transplantation such as skin carcinomas and post-transplant lymphoproliferative disorder (PTLD), occurrence of myeloid neoplasms after solid organ transplantation is relatively rare [2]. Furthermore, myeloid processes in general are more commonly seen in heart and lung rather than liver transplant recipients [3],[4]. As transplant recipients are living longer due to more effective immunosuppressive therapy preventing graft rejection as well as advances in donor–recipient matching, complications such as development of de novo malignancies are becoming more common. Herein, we present a unique case of a 33-year-old man who received an orthotopic liver transplantation in 2021 and then developed MDS followed by transformation into AML. The primary aim of this case study is to describe the clinical presentation and course of these rare but increasingly common complications of orthotopic liver transplantation. In addition, our case represents the third demonstrated case of MDS transforming into AML in an OLT patient in the literature to date [5],[6]. The objective of this case report is to characterize the clinical presentation and course of this rare post-transplant event that may be seen after OLT.
Case Report
Initial hospitalization and post-transplant complications
The patient is a 33-year-old male with a past medical history significant for Diallinas-Amalric syndrome, hypothyroidism, and essential hypertension who originally received an orthotopic liver transplantation in April 2021 for severe alcoholic hepatitis. His postoperative course was marked by numerous complications including renal failure requiring hemodialysis, respiratory failure requiring intubation with multiple episodes of pneumonia, intra-abdominal abscesses requiring drainage, and biliary discontinuity requiring repair. He required a prolonged 7-month hospital stay after his liver transplant due to these complications. His intra-abdominal abscesses were particularly persistent requiring multiple operative interventions to drain them. The patient had several episodes of sepsis postoperatively with blood, intra-abdominal, and lower respiratory tract cultures growing multi-drug resistant (MDR) organisms such as Candida zeylanoides, Enterococcus faecium, Citrobacter freundii, Klebsiella pneumoniae, Bacillus species, and Serratia marcescens. He required tracheostomy and ultimately successful decannulation was performed in October 2021. The patient was started on tacrolimus, mycophenolate mofetil, and prednisone for immunosuppression after his liver transplant but ultimately his prednisone and mycophenolate mofetil were held due to his repeated infections. He was subsequently discharged to a rehabilitation facility in November 2021.
Development of pancytopenia with peripheral blasts
Thereafter, the patient developed leukopenia and neutropenia with intermittent improvement in cell counts after administration of filgrastim. Initially it was thought that the patient’s neutropenia was due to his usage of valganciclovir as the patient developed cytomegalovirus viremia post-transplant and so this medication was held intermittently. However, the patient continued to have bouts of neutropenia and was admitted to the hospital for febrile neutropenia several times over the course of a few months. The patient was followed by the hematology service due to his neutropenia which eventually progressed to pancytopenia with development of peripheral blasts. Flow cytometry on the peripheral blood in September 2022 showed mildly increased myeloid blasts (3.5%) and alteration in the expression of myeloid antigens on the maturing myeloid elements. It also showed increased T-large granular lymphocytes. CD14+ monocytes were 7% of total cells and exhibited aberrant co-expression of CD56. He underwent a bone marrow biopsy the same day which showed increased myeloid blasts (9%), a granulocytic left shift, and alteration in the expression of myeloid antigens on the maturing myeloid elements on flow cytometry analysis of the aspirate. CD56 was again aberrantly co-expressed in a subset of the maturing myeloid population. Bone marrow core biopsy showed a normocellular marrow with maturing trilineage hematopoiesis, granulocytic left shift, and increased megakaryocytes with cytologic atypia. Though increased blasts were detected by flow cytometry, gold-standard morphologic quantification showed no increase in myeloblasts. Fluorescence in situ hybridization (FISH) studies were negative for myelodysplasia-defining abnormalities. Overall, these findings were not diagnostic for myelodysplastic syndrome and at this time additional monitoring with consideration of a repeat bone marrow biopsy in the future was recommended if there was a change in the patient’s clinical state in addition to supportive care for his cytopenias.
Development of myelodysplastic syndrome with excess blasts-2
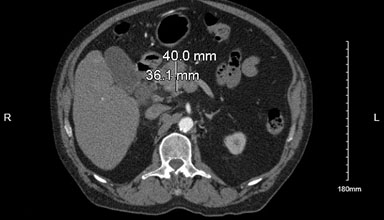
The patient subsequently was thrice admitted to the hospital in November 2022 for worsening abdominal pain, fever, diarrhea, nausea, and vomiting and was found to have leukocytosis with peripheral blasts on his labs. His complete blood count at this time showed a white blood cell count of 48,900/µL with 13% blasts, hemoglobin 8.1 g/dL, and platelets 259,000/µL. BCR-ABL1 quantitative polymerase chain reaction testing was negative. His abdominal computed tomography (CT) scan with oral and intravenous contrast showed a rim-enhancing fluid collection in the rectovesical space with mild wall thickening of the sigmoid colon and rectum. The infectious disease service was consulted, and he was placed on broad spectrum antibiotics. Repeat flow cytometry study of the peripheral blood showed increased myeloid blasts (10%) and IntelliGEN® myeloid next generation sequencing (NGS) panel exhibited one variant of strong clinical significance in the neuroblastoma RAS viral oncogene homolog (NRAS) gene on chromosome 1 (c.181C>A). Cytogenetic analysis exhibited a 46,XY normal male karyotype. He was noted to have an enlarged right axillary lymph node on exam for which he underwent an ultrasound guided biopsy in late November 2022. He additionally underwent a repeat CT guided bone marrow biopsy the same month. His right axillary lymph node biopsy, surprisingly, exhibited minute fragments of tissue with maturing trilineage hematopoiesis consistent with extramedullary hematopoiesis. His bone marrow aspirate showed increased myeloid blasts (10%) and alteration in the expression of myeloid antigens on the maturing myeloid including aberrant co-expression of CD56 on flow cytometry analysis. It was also significant for a cellular marrow with maturing trilineage hematopoiesis, megakaryocytic atypia, and dyspoiesis. The patient met the 2016 World Health Organization (WHO) diagnostic criteria for myelodysplastic syndrome with excess blasts-2 (MDS-EB-2).
Development of refractory anemia with excess of blasts in transformation/acute myeloid leukemia
He was thereafter referred for allogeneic stem cell transplantation but was determined to be a poor candidate due to his various comorbidities. Complete blood count in January 2023 showed a white blood cell count of 23,000/µL with 15% blasts, hemoglobin 7.2 g/dL, and platelets 268,000/µL. Flow cytometry of the patient’s blood revealed 18% myeloblasts in the CD45 dim blast gate, with co-expression of CD34, CD117, HLA-DR, CD38, Dim CD123, CD13, CD33, myeloperoxidase (MPO), and small subset terminal deoxynucleotidyl transferase (TdT), without expression of any T-cell or B-cell lineage markers. This finding was consistent with refractory anemia with excess of blasts in transformation/acute myeloid leukemia (RAEB-T/AML). The patient was recommended for induction chemotherapy with daunorubicin and cytarabine but this was changed to decitabine and venetoclax as his course was complicated by septic shock requiring pressor support presumed due to pelvic fluid collections. He received five days of decitabine. Venetoclax was intermittently held due to the patient’s sepsis and he did not tolerate the full dose; he received 24 out of 28 days in the cycle. The patient did not respond to this regimen and approximately one month later was found to have peripheral blasts in the 45–59% range. Repeat post-induction bone marrow biopsy in March 2023 exhibited increased blasts in a background of multilineage dysplasia as well as a hypercellular bone marrow for age with CD34 positive myeloblasts involving approximately 25–30% of the marrow cellularity (Figure 1A, Figure 1B, Figure 1C, Figure 1D). T cells were present with decreased CD4 to CD8 ratio of 0.27–1 without significant loss or down-regulation of the pan T-cell antigens. He was started on another cycle of decitabine and venetoclax. Unfortunately, the patient did not respond, and he was thereafter admitted twice to the intensive care unit for sepsis and acute hypoxic respiratory failure but he ultimately expired in June 2023.
Discussion
Rarity of development of myeloid processes after orthotopic liver transplantation
We present a unique case of a patient who had received an orthotopic liver transplant developing myelodysplastic syndrome with transformation into acute myeloid leukemia within a short time span. Development of myeloid processes in patients after liver transplantation is relatively rare when compared to patients who have received other organ transplantations such as a heart or lung transplant. Furthermore, AML after liver transplantation is a recent phenomenon with the first cases reported less than three decades ago [7]. Concordantly, there have only been two other cases in the literature which demonstrated MDS transforming into AML in the same liver transplant recipient [5],[6]. The average amount of time between liver transplantation and development of a myeloid neoplasm is variable but according to one review of the literature is approximately three years with a male predominance [8]. Interestingly, our patient was diagnosed with MDS approximately 18 months after receiving his orthotopic liver transplant. This quickly transformed into RAEB-T/AML in a span of two months reflecting the particularly aggressive nature of the patient’s malignancy. Indeed, the time span from organ transplantation to AML tends to be shorter in patients who have received a liver transplant compared to individuals who have received other solid organ transplants such as a renal transplant [9].
Implications of chronic immunosuppression in the post-transplant state
Liver transplant recipients are living longer in part due to more effective immunosuppressive therapy. As life expectancy improves in this patient population, however, the risk of post-transplant malignancy also increases. Patients treated with tacrolimus after their liver transplant have developed myeloid neoplasms according to the literature [3]. Our patient was initially treated with tacrolimus, mycophenolate mofetil, and prednisone for immunosuppression but ultimately had to have the latter two immunosuppressive agents held intermittently due to repeated infections. A fine balance must be struck between the need for immunosuppression in transplant recipients to prevent graft rejection and the necessity of decreasing the risk of adverse effects from such therapy including opportunistic infections and less effective tumor surveillance. One strategy to reduce risk of post-transplant malignancy may be to modulate the patient’s immunosuppression based on their immunosuppressive state which can possibly be gauged through measurement of immunosuppressant drug levels and immune function assays to determine a patient’s “net state of immunosuppression” [8],[10].
Treatment challenges associated with post-solid organ transplant acute myeloid leukemia
According to one review, the median age at the time of diagnosis of AML after solid organ transplant is 50 years of age. Median overall survival was only three months after diagnosis according to the same review [11]. Accordingly, post-solid organ transplant AML tends to portend an aggressive course with a poor prognosis according to the published literature even in patients who have received an allogenic or autologous hematopoietic stem cell transplantation following chemotherapy. Our patient survived for approximately six months after diagnosis of MDS and five months after diagnosis of RAEB-T/AML. He unfortunately was not an optimal candidate for allogeneic stem cell transplantation and succumbed to the disease despite two cycles of decitabine and venetoclax. It is however difficult to say whether hematopoietic stem cell transplantation is an optimal treatment for post-solid organ transplant AML given the relatively limited number of cases that have been published in the literature as well as the heterogeneity of the disease [11].
Variety of presentation of post-liver transplant myeloid processes and its possible implications on treatment
Our patient’s right axillary lymph node biopsy demonstrated maturing trilineage hematopoiesis, a finding consistent with extramedullary hematopoiesis. Extramedullary hematopoiesis in the setting of MDS, especially with trilineage differentiation, is extremely rare [12]. Such a finding has only been sparsely reported in the literature, reflecting the unique nature of our patient’s presentation [13]. The significance of such a finding in regard to prognosis remains unclear due to the limited number of cases that have been published regarding this clinical manifestation of MDS. Furthermore, our patient’s commercial myeloid panel showed one variant of strong clinical significance in the NRAS gene (c.181C>A). Pharmacological blockade of the RAS pathway is actively being researched as a possible treatment option for RAS-driven AML but is not yet commercially available [14]. Indeed, the NRAS gene may be a target for AML treatment as shown in one study in which NRAS mutations disappeared during chemotherapy suggesting a relationship between the mutation and disease status [15]. Yet another study showed that there was no significant difference between survival and remission in AML patients with the NRAS mutation and those without the mutation [16]. Further research is needed to determine both the optimal immunosuppressive regimen in solid organ transplant recipients to prevent development of secondary malignancies as well as the treatment regimen that will offer the best chance of remission.
Conclusion
Post-liver transplant myeloid neoplasms are becoming more common as transplant recipients are living longer with more effective immunosuppression and better donor–recipient matching. Our case demonstrates a unique phenomenon of MDS transforming into AML after liver transplantation with only two other cases in the literature showing such a transformation in the same liver transplant recipient. The patient was on chronic immunosuppressive therapy after his transplant mostly with tacrolimus and this likely played a role in the development of his myeloid neoplasm although further research is needed in this area to determine the optimal immunosuppressive regimen to prevent post-transplant malignancies in this unique patient population. The ability to determine a patient’s “net state of immunosuppression” in the future could therefore provide an adequate clinical status for a patient so that their immunosuppressive therapy is modulated accordingly. Unfortunately, our patient was not a candidate for allogeneic stem cell transplantation due to his various comorbidities and poor functional status and he succumbed to the disease despite two cycles of decitabine and venetoclax approximately six months after being diagnosed with MDS which eventually transformed into AML. Although this patient’s cytogenetics were unremarkable, he did have a variant of strong clinical significance in the NRAS gene which likely played a role in the pathogenesis of his myeloid processes. His case also demonstrated extramedullary hematopoiesis in the form of his axillary lymph node biopsy showing maturing trilineage hematopoiesis, a rare finding of uncertain significance in MDS which could possibly reflect the aggressive nature of the patient’s disease. Post-liver transplant myeloid neoplasms tend to be heterogeneous in nature and thus unfortunately a “one size fits all” treatment regimen is not a viable option for this patient population. Targeted therapy for RAS-driven AML is being actively researched and could be beneficial in this rare post-transplant complication which tends to portend a poor prognosis. Due to the varied presentation of this unique phenomenon that may be seen after OLT, further research on post-liver transplant myeloid processes is needed to provide appropriately tailored treatment regimens to affected patients. Clinicians should thus approach patients affected by post-liver transplant myeloid neoplasms cautiously and with an open mind.
REFERENCES
1.
Wu B, Ingersoll K, Jug R, et al. Myeloid neoplasms following solid organ transplantation: Clinicopathologic studies of 23 cases. Am J Clin Pathol 2017;149(1):55–66. [CrossRef]
[Pubmed]

2.
Morton LM, Gibson TM, Clarke CA, et al. Risk of myeloid neoplasms after solid organ transplantation. Leukemia 2014;28(12):2317–23. [CrossRef]
[Pubmed]

3.
Liu M, Liu J, Liu L, et al. A case report of acute myeloid leukemia after liver transplantation. Acta Haematol 2013;129(4):225–8. [CrossRef]
[Pubmed]

4.
Camós M, Esteve J, Rimola A, et al. Increased incidence of acute myeloid leukemia after liver transplantation? Description of three new cases and review of the literature. Transplantation 2004;77(2):311–3. [CrossRef]
[Pubmed]

5.
Zhang GS, Dai CW, Peng HL, Xu YX, Pei MF. Myelodysplastic syndrome with transformation to acute monocytic leukemia with FLT3-ITD mutation following orthotopic liver transplantation. Leuk Res 2006;30(7):908–10. [CrossRef]
[Pubmed]

6.
Kourelis TV, Boruchov A, Hull D, et al. Acute myeloid leukemia following solid organ transplantation: Case report and comprehensive review. Conn Med 2012;76(3):151–4.
[Pubmed]

7.
Thalhammer-Scherrer R, Wieselthaler G, Knoebl P, et al. Post-transplant acute myeloid leukemia (PTAML). Leukemia 1999;13(3):321–6. [CrossRef]
[Pubmed]

8.
Jiang N, Li H, Wang GS, et al. Acute leukemia, a rare but fatal complication after liver transplantation. Leuk Res 2009;33(10):1349–51. [CrossRef]
[Pubmed]

9.
Cho YU, Chi HS, Park CJ, et al. Two cases of post-liver transplant acute myeloid leukemia in Korean adults: Review of bibliographies and comparison with post-renal transplant acute myeloid leukemia. Ann Hematol 2008;87(6):513–4. [CrossRef]
[Pubmed]

10.
Roberts MB, Fishman JA. Immunosuppressive agents and infectious risk in transplantation: Managing the “net state of immunosuppression.” Clin Infect Dis 2021;73(7):e1302–17. [CrossRef]
[Pubmed]

11.
Rashidi A, Fisher SI. Acute myeloid leukemia following solid organ transplantation: Entity or novelty? Eur J Haematol 2014;92(6):459–66. [CrossRef]
[Pubmed]

12.
Wang C, Shi Y. Extramedullary hematopoiesis in myelodysplastic syndromes: A systematic literature review. Hemato 2022;3(3):569–73. [CrossRef]

13.
Hancock JC, Prchal JT, Bennett JM, Listinsky CM. Trilineage extramedullary myeloid cell tumor in myelodysplastic syndrome. Arch Pathol Lab Med 1997;121(5):520–3.
[Pubmed]

14.
Marín-Ramos NI, Balabasquer M, Ortega-Nogales FJ, et al. A potent isoprenylcysteine carboxylmethyltransferase (ICMT) inhibitor improves survival in ras-driven acute myeloid leukemia. J Med Chem 2019;62(13):6035–46. [CrossRef]
[Pubmed]

15.
Jeong JH, Park SH, Park MJ, et al. N-ras mutation detection by pyrosequencing in adult patients with acute myeloid leukemia at a single institution. Ann Lab Med 2013;33(3):159–66. [CrossRef]
[Pubmed]

16.
Casey G, Rudzki Z, Roberts M, Hutchins C, Juttner C. N-ras mutation in acute myeloid leukemia: Incidence, prognostic significance and value as a marker of minimal residual disease. Pathology 1993;25(1):57–62. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Ravi Upadhyay - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Manali Shah - Conception of the work, Design of the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Virian Serei - Acquisition of data, Analysis of data, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Dayna Panchal - Conception of the work, Design of the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Ankit Shah - Conception of the work, Design of the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guaranter of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was not obtained from the patient as the patient is deceased and no patient identifiers were used in the publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2024 Ravi Upadhyay et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.