|
| Case Report | ||||||
| Concurrent treatment of metastatic breast and metastatic renal cell carcinoma: A case report | ||||||
| Sarah Jane Zardawi1, Mathew Kattathra George2 | ||||||
| 1MBBS B Med Sci, Advanced Trainee, Calvary Mater Newcastle, Calvary Mater Hospital, Waratah, 2298, NSW, Australia 2DM FRACP MSc, Adjunct Associate Professor, Staff Specialist in Medical Oncology and General Medicine, North West Cancer Center, Tamworth Rural Referral Hospital, NSW, Australia | ||||||
| ||||||
| [HTML Abstract]
[PDF Full Text][Print This Article] [Similar articles in PubMed][Similar articles in Google Scholar] |
| How to cite this article |
| Zardawi SJ, George MK. Concurrent treatment of metastatic breast and metastatic renal cell carcinoma: A case report. J Case Rep Images Oncology 2018;4:100054Z10SZ2018. |
| ABSTRACT | ||||||
|
Introduction: Breast and renal carcinomas are common malignancies, with an increasing number of well-tolerated targeted therapies. Case Report: We describe a case of concurrent, synchronous, metastatic breast and renal carcinomas where diagnosis was achieved after biopsy of two incongruous metastatic sites. The patient has been successfully treated with targeted therapies, exemestane and sunitinib, and later anastrozole and pazopanib, with radiological improvement and resolution of symptoms. Conclusion: Literature review of cases of antecedent, synchronous and metachronous breast and renal cancers (multiple malignancies), did not reveal increased risk of developing renal cancer after breast cancer, or of breast cancer after renal cancer. Cases of multiple breast and renal cancers appear to occur at any time with out clear reasons for their occurrence. This case demonstrates the importance of appropriate investigation and accurate diagnosis of synchronous malignancies in patients who may be candidates for treatment targeted therapies. As clinical experience of concurrent use of targeted therapies grows, including trials for potential additive benefits of using targeted agents in combination, we will be able to offer improved treatment options for patients with both single and multiple malignancies. Keywords: Multiple malignancies, Targeted therapies | ||||||
| INTRODUCTION | ||||||
|
Metastatic breast and renal carcinomas have an increasing number of well-tolerated, targeted therapies. This has made it possible to effectively treat patients whom otherwise might not have been considered for anti-cancer treatment, including patients with more than one advanced malignancy. This case report explores a patient with concurrent metastatic breast and renal carcinomas who has been treated successfully with two targeted therapies with radiological improvement and resolution of symptoms. | ||||||
| CASE REPORT | ||||||
|
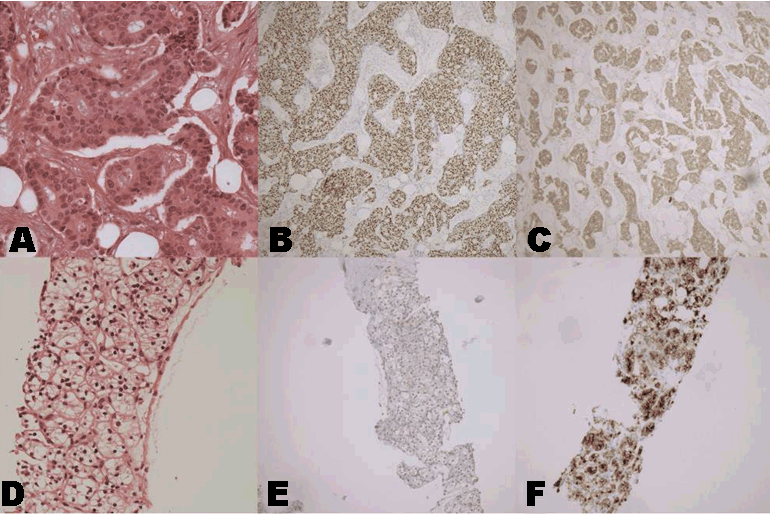
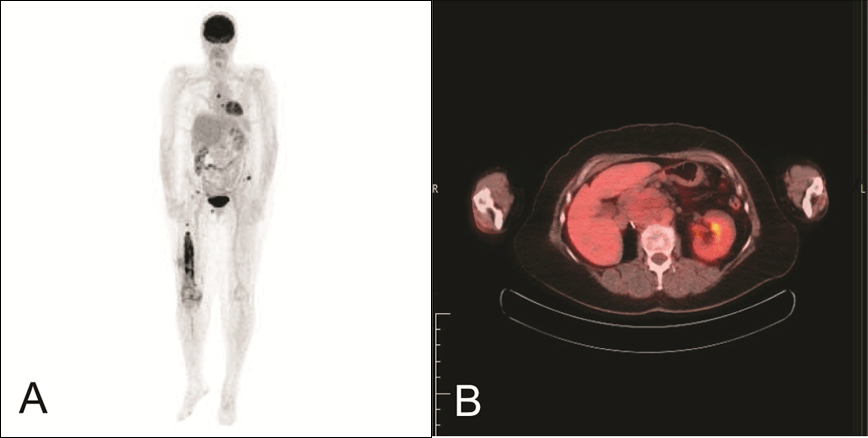
A 69-year-old female was incidentally noted to have a suspicious femoral lesion during elective right total knee replacement. This was on a background of a right breast carcinoma treated with mastectomy 35 years prior; a left breast carcinoma treated with partial mastectomy, adjuvant radiation and adjuvant tamoxifen 14 years prior; and a right clear cell renal carcinoma treated with nephrectomy nine years prior. The femoral lesion was biopsied, revealing metastatic oestrogen- and progesterone-receptor positive adenocarcinoma consistent with her prior hormone receptor positive left breast carcinoma (Figure 1 A-C). Staging computed tomography (CT) and FDG positron emission tomography (PET) identified multiple PET-avid lesions consistent with metastases in the pelvis, acetabulum, right femur, sternum, thoracic fifth and eighth vertebrae, and lumbar fifth vertebrae (Figure 2A). There was also a large, non PET-avid, pathological retro caval node, which was not in keeping with a diagnosis of metastatic breast carcinoma (Figure 2B). Biopsy of this node showed metastatic clear cell renal carcinoma consistent with her prior renal carcinoma (Figure 1 D-F). The patient received palliative radiotherapy to the sternum, thoracic spine, lumbar spine, left ilium and retro caval lymph nodes. She was initially commenced on exemestane and sunitinib and subsequently changed to anastrozole and pazopanib due to gastrointestinal adverse effects. Restaging CT scan, bone scan, and PET scan have shown radiological response with reduction in size and PET avidity of her metastases. This response was durable for 24 months and associated with good symptom control and functional status. At time of commencement of therapy there was no subsidized access to cyclin-dependent kinase 4/6 inhibitors. | ||||||
|
| ||||||
| ||||||
| ||||||
| ||||||
DISCUSSION | ||||||
|
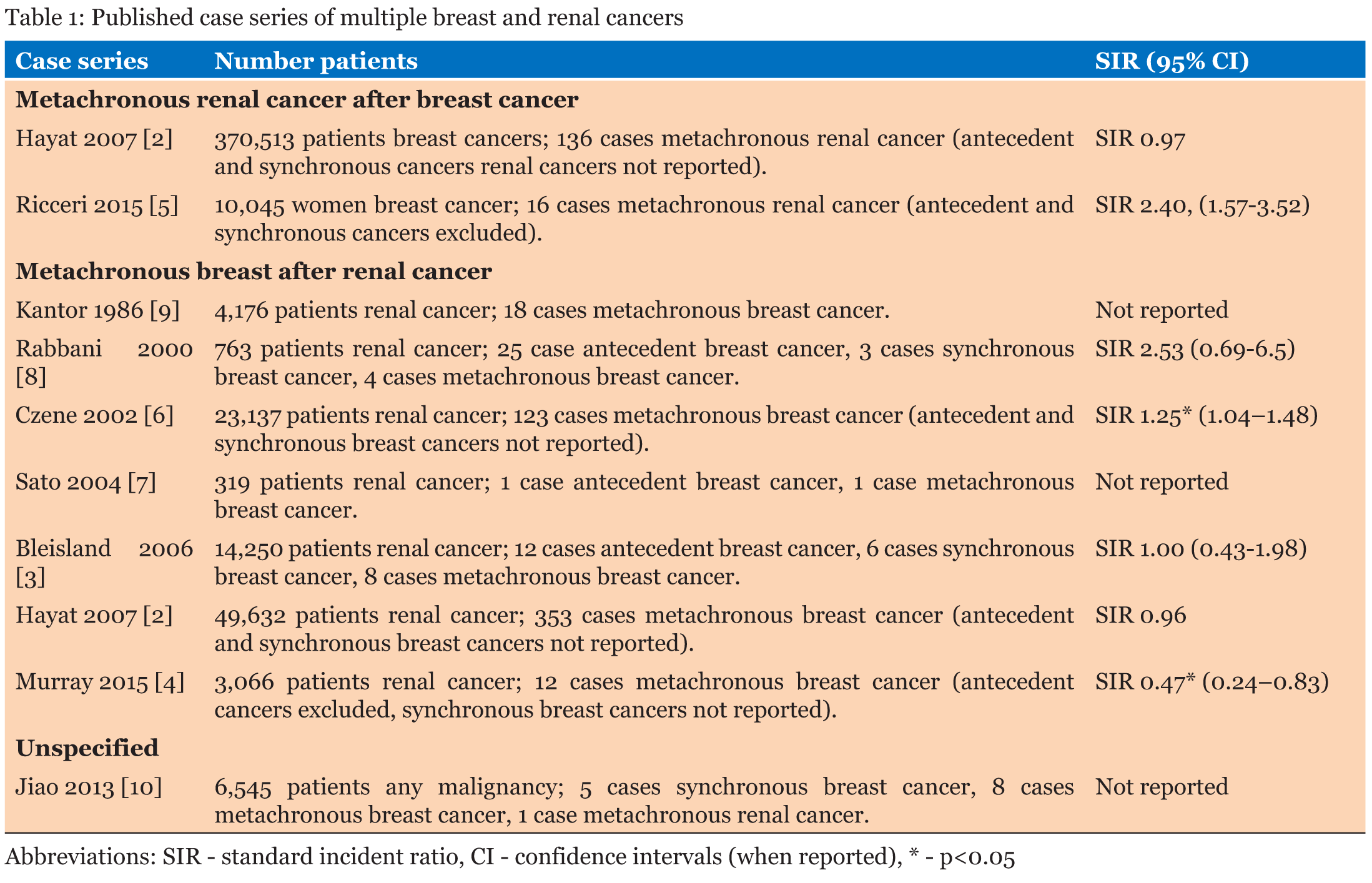
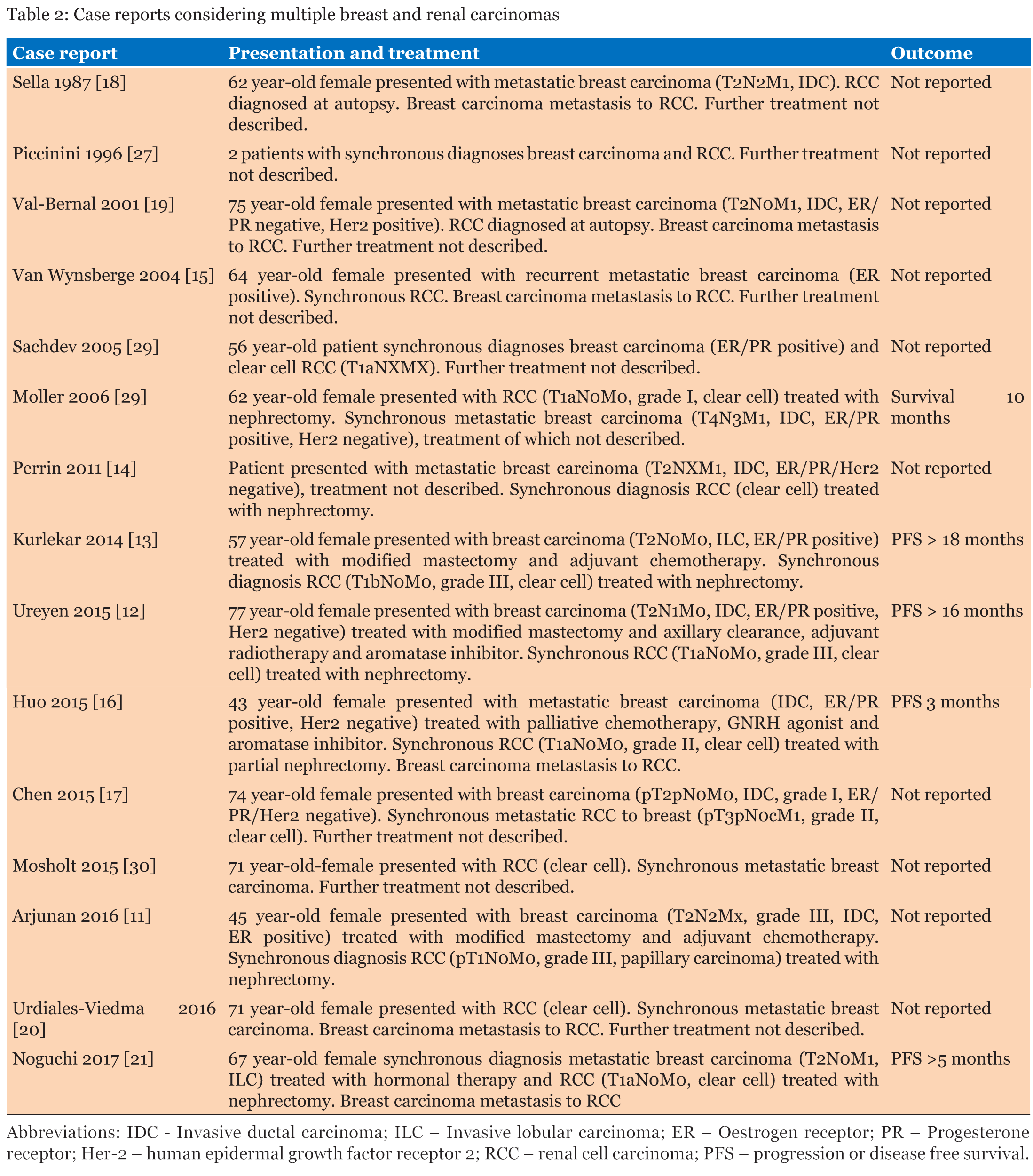
Multiple malignancies are cases of multiple, pathologically distinct malignancies occurring in the one individual. The malignancies are described according to the time of diagnosis relative to the malignancy of interest. Antecedent malignancies occur at least 6 months prior to; synchronous malignancies are detected within six months; and metachronous malignancies are detected greater than six months after the malignancy of interest [1],[2],[3],[4]. Antecedent, synchronous and metachronous malignancies are collectively referred to as multiple malignancies. Our case documents synchronous metastatic breast and renal carcinomas. The following discussion is based on a literature review using the PubMed database with the search terms breast carcinoma, breast cancer, renal carcinoma, renal cancer multiple malignancy, antecedent malignancy, synchronous malignancy and metachronous malignancy, as well as review of the references cited in articles retrieved through this search. Both full text articles and abstracts were included. There are many instances of multiple malignancies involving breast and renal cancer, with previously reported case series listed in Table 1 [2], [3], [4], [5], [6], [7], [8], [9], [10]. However, despite these reported occurrences these series do not show an increased risk of developing renal cancer after breast cancer (standard incident ratio (SIR) 0.97–2.40) [2],[5] or of developing breast cancer after renal cancer (SIR 0.47–2.53) [2], [3], [4], [6], [7], [8], [9] compared to the background population risk of developing either malignancy. The time interval between malignancies in our patient was 26 years between right breast and renal cancer, and 5 years between the left recurring breast and renal cancer. This is similar to the median published time to the development of breast cancer after renal cancer of 5.5–24.2 years [4],[7]. Whilst this is the reverse order of malignancies to our case it highlights that metachronous malignancies can develop at any time. Published case reports of patients with synchronous breast and renal carcinomas and are described in Table 2 [11], [12], [13], [14], [15], [16], [17], [18], [19], [20], [21], [22], [23], [24], [25], [26], [27], [28], [29], [30]. Review of these cases show that it was more common to present with breast cancer (either early or advanced stage) and be diagnosed with a synchronous renal cancer [11], [12], [13], [14], [15], [16], [17], [18], [19]. When reported, the renal cell cancer was often a low grade and low stage cancer [11], [12], [13], [14], [15], [16], [17], or an incidental autopsy finding [18], [19]. Interestingly, there were several cases of breast cancer metastasizing to a renal cancer, known as tumour-to-tumour metastases [15], [16], [17], [18], [19], [20], [21], but no cases of renal cancer metastasizing to a breast cancer. Further, there are no cases like ours that report synchronous metastatic breast and metastatic renal cancers. Age is a known risk factor for multiple malignancies with one case series of renal cancers documenting that patients with synchronous or metachronous malignancies of any type were five years older than those without a second malignancy (P=0.0072) [8]. Otherwise, the development of second malignancies is thought to be dependent upon lifestyle factors, previous cancer treatments and genetic susceptibilities. For breast and renal cancers, there are common life style risk factors of cigarette smoking and obesity [5],[22], [23] but the treatments used for breast and renal cancer are not associated with an increased risk of the other malignancy [24], [25], [26], nor are there common inherited genetic conditions. Despite an absence of clear causative reasons for multiple malignancies, as treatment of cancer and other diseases improves it is likely that the incidence of patients with multiple malignancies will increase. Our patient was commenced on the targetted therapies, exemestane and sunitinib, and subsequently anastrozole and pazopanib for treatment of her metastatic breast and renal carcinomas. Exemestane and anastrozole are aromatise inhibitors that prevent the conversion of circulating oestrogen pre-cursors to oestrogen to reduce exposure of growth promoting oestrogen to breast cancer cells [31]. Sunitinib and pazopanib are tyrosine kinase inhibitors that prevent the activation of vascular endothelial growth factor receptors, platelet derived growth factors and stem cell factor receptor to affect the survival, proliferation, vascularization and metastasis of renal cancer cells [32]. Whilst these therapies have established efficacy for treatment of their respective malignancies, current phase II clinical trials are testing combined use of targeted therapies for potential increased efficacy in post menopausal breast cancer. These trials include the use of pazopanib with an aromatase inhibitor for the neoadjuvant treatment of stage II-III breast cancer [33], and with an aromatase inhibitor following development of resistance in metastatic breast cancer [34]. Such studies may explain why our patient has had such a significant response to treatment (noting that she also had palliative radiotherapy to most sites of disease), as well as offer improved treatment options for patients with both single and multiple malignancies. Previously multiple malignancies have previously been associated with poorer outcomes. Two case series of renal cancers found that patients with antecedent or synchronous cancers had 5-year survival rates of approximately 30% compared with 50% for patients without a second malignancy [3]. Sato et al also demonstrated that an antecedent or synchronous tumour, like a high pathological stage, was a strong independent poor prognostic factor for overall survival in patients with renal cell cancer [7]. Further, the median survival time was vastly worse for synchronous cancers than for metachronous cancer (3.8 years versus 17.3 years, p<0.05) [7], potentially due to the challenges of treating two malignancies at the same time. Fortunately, our patient has had durable response to treatment for 24 months, which may suggest improved outcomes for these patients with targeted therapies. | ||||||
| CONCLUSION | ||||||
|
This case demonstrates the importance of appropriate investigation and accurate diagnosis of synchronous malignancies in patients who may be candidates for treatment with multiple targeted therapies, which is a situation that is anticipated to become more common in the future due to improving health outcomes and cancer therapies. As clinical experience of concurrent use of targeted therapies grows, including trials for potential additive benefits of using targeted agents in combination, we will be able to offer improved treatment options for patients with both single and multiple malignancies. | ||||||
| REFERENCES | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
| Acknowledgements
Brianna Wright, Christopher Renaud, Susan Pendlebury. |
| Author Contributions
Sarah Jane Zardawi – Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Mathew Kattathra George – Substantial contributions to conception and design, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of Submission
The corresponding author is the guarantor of submission. |
|
Source of Support
None |
|
Consent Statement
Written informed consent was obtained from the patient for publication of this case report. |
|
Conflict of Interest
Author declares no conflict of interest. |
|
Copyright
© 2018 Sarah Jane Zardawi et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|