|
|
Case Series
| ||||||
| Severe neurological side effects associated with ipilimumab: A case series | ||||||
| Muriel Richard1, Emilie Gerard1, Philippe Casenave1, Sorilla Prey1, Anne-Pham Ledard1, Diane Mermin1, Aurélia Gey1, Caroline Dutriaux1 | ||||||
|
1Department of Dermatology, National Reference Center for Rare Skin Disorders, University Hospital of Bordeaux, France
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article: |
| Richard M, Gerard E, Casenave P, Prey S, Anne-Pham L, Mermin D, Gey A, Dutriaux C. Severe neurological side effects associated with Ipilimumab: A case series. J Case Rep Images Oncology 2017;3:29–34. |
|
ABSTRACT
|
|
Introduction:
Ipilimumab (IPI) is a T cell-potentiating monoclonal antibody used since 2011, directed against cytotoxic T-lymphocyte antigen-4 (CTLA-4) to promote anti-tumoral immunity. In phase II and III trials, IPI was shown to be the first agent to improve overall survival (OS) in advanced melanoma patients, regardless of previous treatment. Neurological immune-related adverse events (irAEs) associated with IPI are rare, multiple and often badly known. We report four new cases of severe neurological events during and after IPI treatment.
Case Series: We report four cases of metastatic melanomas with neurological irAEs induced by IPI in our dermatology department, between November 2014 and August 2015. Our four patients treated with IPI developed chronic inflammatory demyelinating polyneuropathy (CIDP), peripheral neuropathy, meningoencephalitis and aseptic meningitis respectively. In all, IPI was discontinued due to toxicity. High-dose intravenous steroids were given to all patients except in the patient who experienced aseptic meningitis. The one with CIDP also received intravenous immunoglobulins and plasmapheresis, without clinical improvement. Conclusion: These four cases enrich the knowledge on neurological IPI induced-irAEs whose spectrum is wide and symptoms sometimes atypical. Early diagnosis and appropriate treatment are essential to minimize severe complications. Regarding our patients, these severe neurological irAEs were not predictive of an anti-tumoral response. | |
|
Keywords:
Aseptic meningitis, Chronic inflammatory demyelinating polyneuropathy, Ipilimumab, Metastatic melanoma, Neurologic immune-related adverse events,
Peripheral neuropathy
| |
|
INTRODUCTION
|
|
Cutaneous melanoma is the most aggressive form of skin cancer. TNM melanoma and anatomic stages was defined by the seventh version of the American Joint Committee on Cancer (AJCC) in 2009 [1] (Table 1). To treat advanced melanomas, the first step is to identify patients with B-RAFV600 mutation by molecular analysis of tumor tissue. If the tumors cells harbor a B-RAF mutation, targeted therapies can be used, such as B-RAF inhibitors, alone or in combination with a MEK inhibitor. Tumors cells without B-RAF mutation, called B-RAF wild-type, receive immunotherapy such as IPI or anti-PD1 as first-line treatment. Immunomodulation with the anti-CTLA-4 monoclonal antibody IPI has been shown to improve OS in previously treated and treatment-naive patients with unresectable stage III or IV melanoma [2][3] . Blockage of CTLA-4 signaling with IPI prolongs T cell activation and restores T cell proliferation. It causes immune effects on various organ systems, leading to irAEs. IPI-associated irAEs are common and typically low grade and manageable, but can also be serious and life threatening. Skin and gastrointestinal tract are most frequently affected [4] while hepatic, endocrine, and neurological events are less common. The incidence of neurological irAEs involving central or peripheral nervous system in patients treated with IPI in phase II and III trials is estimated to be around 0.1%, with no reported grade 3–4 events. However, one death was recorded in the phase III trial secondary to Guillain-Barre syndrome [2][5][6][7]. Myasthenia gravis-like symptoms have also been reported in <1% of patients who received higher doses of IPI in clinical trials. Similarly, sensorimotor neuropathy [8], inflammatory myopathy [9], aseptic meningitis with cerebrospinal fluid lymphocytosis [10], severe meningoradiculoneuritis [11], myasthenia [12][13], transverse myelitis [12], CIDP [12], Guillain-Barre syndrome [14], inflammatory enteric neuropathy with severe constipation [15] and posterior reversible encephalopathy syndrome (PRESS) [16] have been described. With proper management, most irAEs resolve within a relatively short time. Our aim is to report four new cases of neurological adverse events. |
|
CASE SERIES
|
|
Case 1 |
| A 71-year-old male with stage IV melanoma, B-RAF wild-type, received three cycles of dacarbazine, then six cycles of carboplatine-paclitaxel because of progression of his underlying disease, allowing to stabilize his disease. After the second infusion, distal sensorimotor troubles, grade 1–2, appeared, first to the feet including weakness, paresthesias and decrease of sensibility with then progression to the upper limbs. As these symptoms were stable, he received three more infusions with a 30% dose reduction. However, a few months later, his treatment was switched to IPI every three weeks because of this neurotoxicity. Two weeks after the first infusion, the neurological symptoms rapidly worsened with decreased distal sensitivity, permanent paresthesia, walking troubles and sphincter dysfunction with urinary incontinency. Neurological examination revealed decreased sensation to light touch, pinprick and proprioception on the distal members, bilateral distal muscle weakness with negative tendon reflexes. Cranial nerves were normal. Rapidly, he lost distal muscle strength and all sensitivity from toes to ankles and from fingers to wrists. Cerebrospinal fluid (CSF) showed high proteins level (2, 72g/L) without malignant cells. Other laboratory tests, including complete blood count, viral, bacterial tests and screening for autoantibodies were negative (anti-MAG, anti-ganglioside). Electrophysiological studies demonstrated no motor response in the lower limbs, prolonged distal motor latencies with a slowing down of all motor and sensitive conduction velocities. There were also signs of denervation in both upper and lower extremities. No neuromuscular biopsy was performed. These findings and the subacute evolution were suggesting of CIDP. IPI was withheld after the first two infusions, and treatment with intravenous immunoglobulins (IVIg) at a dose of 0, 4 g/kg/daily for five days every four weeks, was begun in association with 30 mg of oral prednisone with an initial improvement. Two months later, after a worsening of the neurological involvement, IVIg were stopped and Solu-Medrol infusions (1 g) were begun coupled with plasmapheresis. Both distal motor and sensory symptoms improved after five sessions. Paresthesias were persistent. Plasmapheresis was maintained twice a week during four weeks but their efficacy quickly waned and the symptoms worsened. Thus, this treatment was also stopped. At this point, only oral prednisone was still given at the dose of 40 mg/day. In the meantime, a worsening of his hepatic metastatic lesions was noticed, and a conventional chemotherapy by fotemustine was started as third line without benefit. No further melanoma specific treatment was administrated. The patient died one month later secondary to a fast-deterioration of his CIDP complications. |
| Case 2 |
|
A 70-year-old female with stage IV melanoma, B-RAF wild type, was first treated with IPI. Only three infusions out of four were given because of colitis which improved with high-dose prednisone and one infusion of infliximab 5 mg/kg. The tumor assessment was stable. Eight weeks later, the patient noticed blurry vision with occasional left eye ptosis, proximal legs weakness and had gait balance disorder. Urination and defecation were difficult. These troubles appeared although she was on high-doses prednisone for the colitis. Ophthalmological examination was normal. Motor strength testing was symmetric, decreased on the four members with difficulties to stand up. Sensory examination showed decreased sensation for fine touch and proprioception from the sacrum down, with a frank medullary level in T12. Tendon reflexes were absent without a Babinski sign. There was neither disorder of the sphincter contractility, nor loss of genital sensibility but genital reflexes were absent. Brain magnetic resonance imaging (MRI) scan was normal without medullary compression. Usual blood tests, including creatine phosphokinase (CPK) and lumbar puncture analyses were normal with no anti-neuronal antibodies. Nerve conduction studies (NCS) with electromyography (EMG) were suggestive of severe distal sensorimotor neuropathy without argument for a polyradiculoneuropathy. No neuromuscular biopsy was performed. Laboratory tests for myasthenia gravis were negative. Uro-dynamic analysis showed a normal curve but a residue of 100 ml in the bladder. Given the clinical picture and her lab results, the IPI was deemed to be the most likely cause for her symptoms. Treatment by oral steroids was started, 1 mg/kg for an additional month, with slow dose tapering. The neurological examination few months later revealed an improvement in strength, sensitivity, vision and vesical disorders. Unfortunately, six months after the last IPI infusion, a progression of her lung metastases was assessed. With a follow-up of nine months, she had almost totally recovered. |
| Case 3 |
|
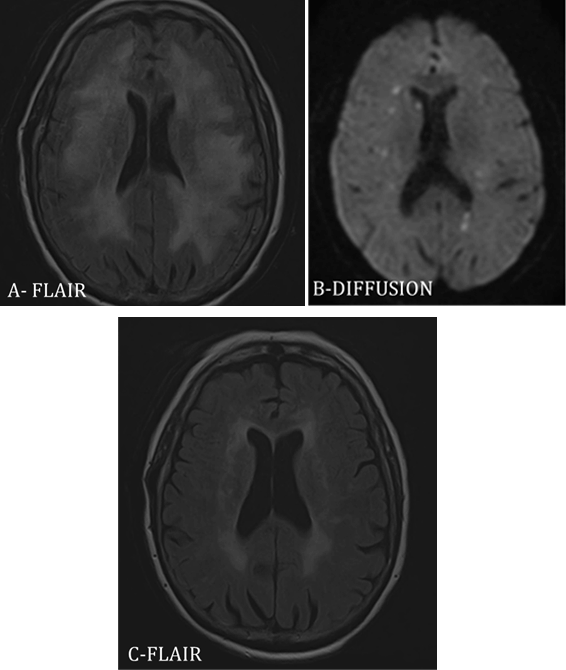
A 76-year-old female had been diagnosed with a mucosal metastatic melanoma. She received IPI as a first line treatment. After two infusions appeared psychomotor slowing down and urinary symptoms. After the third infusion were noted walking difficulties and falls, ataxia and apraxia and urinary incontinence. The fourth infusion of IPI was not done. The examination showed a moderate cerebellum syndrome with ataxia. Tendons reflexes were exaggerated without Babinski sign. There was no loss of strength or sensibility. The urinary incontinence persisted. Usual blood analyses and explorations of hypothalamo-pituitary axis were normal. Lumbar punctures revealed an inflammatory fluid with predominantly lymphocytic cells (141 cells/mm3), increased protein level (1 g/L) and normal sugar level but no malignant cells. Anti-neuronal antibodies were absent. No infections agent was found in the CSF. Brain MRI scan revealed leukoencephalopathy (Figure 1A), multiple multifocal recent ischemic defects (Figure 1B), with small-caliber arteries enhancing after injection, suggesting vasculitis of the small vessels. Electroencephalograms showed specific diffuse brain suffering. Medullary MRI scan was normal. Meningoencephalitis induced by IPI was suspected and the infusions were withheld. A course of high-dose intravenous methylprednisolone was started, 1 g daily for five days then switched for 1 mg/kg oral prednisone, with slow dose tapering, with significant improvement in both motor and vigilance symptoms. However, walking instability and memory disorders worsened. Neurological examination two months later showed a partial improvement of all symptoms except for her urinary incontinence. The lumbar punctures revealed a persistent inflammatory fluid. Brain MRI scan showed a significant decrease of T2 hypersignals (Figure 1C), and only few recent ischemic defects. Six months after the last IPI infusion, the tumoral assessment was consistent with stable disease. |
| Case 4 |
|
A 77-year-old male with stage IV melanoma, B-RAF wild type, was first treated with IPI. Three weeks after the fourth infusion, he developed headache and vomiting associated with severe fatigue and pyrexia. Usual blood analyses revealed inflammation (CRP 330 mg/l). All tests exploring the hypothalamo-pituitary axis showed decreased hormone levels. The lumbar puncture revealed a small inflammatory CSF with predominantly lymphocytic cells (9/mm3), and increased proteins level (0, 56 g/L) but no malignant cells. Computed tomography scan showed lungs metastases were stable. There were no brain metastases on the MRI, nor inflammation of the pituitary gland or infundibulum. These results were suggesting of aseptic meningitis and panhypopituitarism induced by IPI. Symptoms significantly improved with hydrocortisone 60 mg daily. Amoxicillin plus clavulanic acid (1 gm three times a day) was started in the hypothesis of frontal sinusitis. The patient partially recovered but he complained of a painful increase of the testicular volume with no urinary dysfunction or infection. Testicular echography was consistent with bilateral orchiepididymitis. In this context of autoimmunity, the role of IPI as a causative agent was assessed. One month later, all symptoms disappeared, and his cancer was stable. However, a pulmonary progression was noticed four months after the last IPI infusion, and second line treatment with PD1 blocker (pembrolizumab) was started allowing tumor stabilization without new neurological adverse events. |
|
|
|
DISCUSSION
|
|
Melanoma is an immunogenic malignant tumor. IPI-associated irAEs such as skin, gastrointestinal, joint, endocrine or hepatic disorders are more common than neurological events. Peripheral nervous system symptoms may be explained by a common embryonic origin of the melanocytes and Schwann cells, both derived from neural crest, sharing surface molecules (such as MAG and the gangliosides GM3, GD3, GM2 and GD2) with immunogenic similarities. By a cross reaction called molecular mimicry, immune response directed against the tumor might also be responsible for the destruction of similar antigens in Schwann cells, causing neurological symptoms [17]. Central involvement is less known but a few authors have assessed the potential role of pro-inflammatory interleukin IL1 and IL17 in it [11][18]. The role of IL6 has also been studied [12]. Neuropathies have been reported in melanoma patients vaccinated with melanoma cell lysates or receiving monoclonal anti-GD2 antibodies, or interferon alpha-2b [19][20]. They have also been linked to paraneoplastic neurological syndromes (PNS). In our 4 cases, IPI was discontinued due to the development of severe, grade 3–4 adverse events. Immunoglobulins and plasmapheresis was initiated in the patient with CIDP without significant clinical efficacy, which may be explained by a delayed diagnosis. In contrast, the patient with polyneuropathy and meningoencephalitis did better after discontinuation of IPI, and treatment with high-dose intravenous steroids. To our knowledge, this is the second case of CIDP to be reported in literature. In 2014, Liao and al. [12] published the first case, that developed after two IPI infusions and improved significantly after seven courses of plasmapheresis. In contrast, our patient already suffered from chemo-induced neuropathy and did not improve with treatments. First line treatment for grade 3–4 neurological symptoms is intravenous corticosteroids. In non-steroids responsive patients, other treatments should be tried including intravenous immunoglobulin, plasma exchange or other immunosuppressive agents. IPI should be stopped [21]. A remarkable association between skin auto-immunity such as vitiligo and a favorable outcome has been reported, especially in melanoma patients treated with novel immunotherapeutic agents [22]. However, in the case of our patients, these neurologic irAEs were not associated with an anti-tumoral response, since melanoma assessments showed progression at week-16 for the patient with CIDP and at week-24 for the one with neuropathy. The patients with meningoencephalitis and aseptic meningitis remained stable at least 24 weeks. When the first patient had progression of his melanoma, a switch for a PD1 blocker was suggested but finally rejected given the same expected irAEs. As such, chemotherapy was instead started. The patient with aseptic meningitis was started on pembrolizumab six months after his last IPI infusion with good tolerance. |
|
CONCLUSION
|
|
Neurological immune-related adverse events (irAEs) under ipilimumab (IPI) should be suspected at the earliest to start the appropriate management. The question nowadays is to assess the potential risk of PD1 blockers administration after IPI induced neurological toxicity. At the dawn of a new era of biotherapeutic regimens, another question to consider is whether these toxicities will be more severe than those experienced on monotherapy. |
|
REFERENCES
|
|
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Muriel Richard – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Emilie Gerard – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Philippe Casenave – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Sorilla Prey – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Anne-Pham Ledard – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Diane Mermin – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Aurélia Gey – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Caroline Dutriaux – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Muriel Richard et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |